HIPAA compliance is critical for billing teams handling Protected Health Information (PHI). Mistakes like sending statements to the wrong patient or failing to secure sensitive data can lead to fines up to $1.5 million annually, damage your reputation, and erode patient trust. To avoid these risks, training your billing staff is essential.
Here’s how to ensure compliance:
- Assess Knowledge: Use quizzes and scenario-based tests to identify gaps in HIPAA understanding.
- Review Workflows: Audit billing processes to spot risks like unsecured devices or improper PHI handling.
- Create Tailored Training: Teach the "minimum necessary" standard, role-based access, and breach response procedures.
- Use Interactive Methods: Include exercises like phishing simulations and short, focused modules.
- Document Everything: Maintain detailed training records to meet regulatory requirements.
- Implement Policies: Develop clear billing-specific HIPAA policies for PHI access, workstation security, and remote work.
- Monitor and Update: Conduct regular audits, offer refresher courses, and adapt training to new tools or regulations.
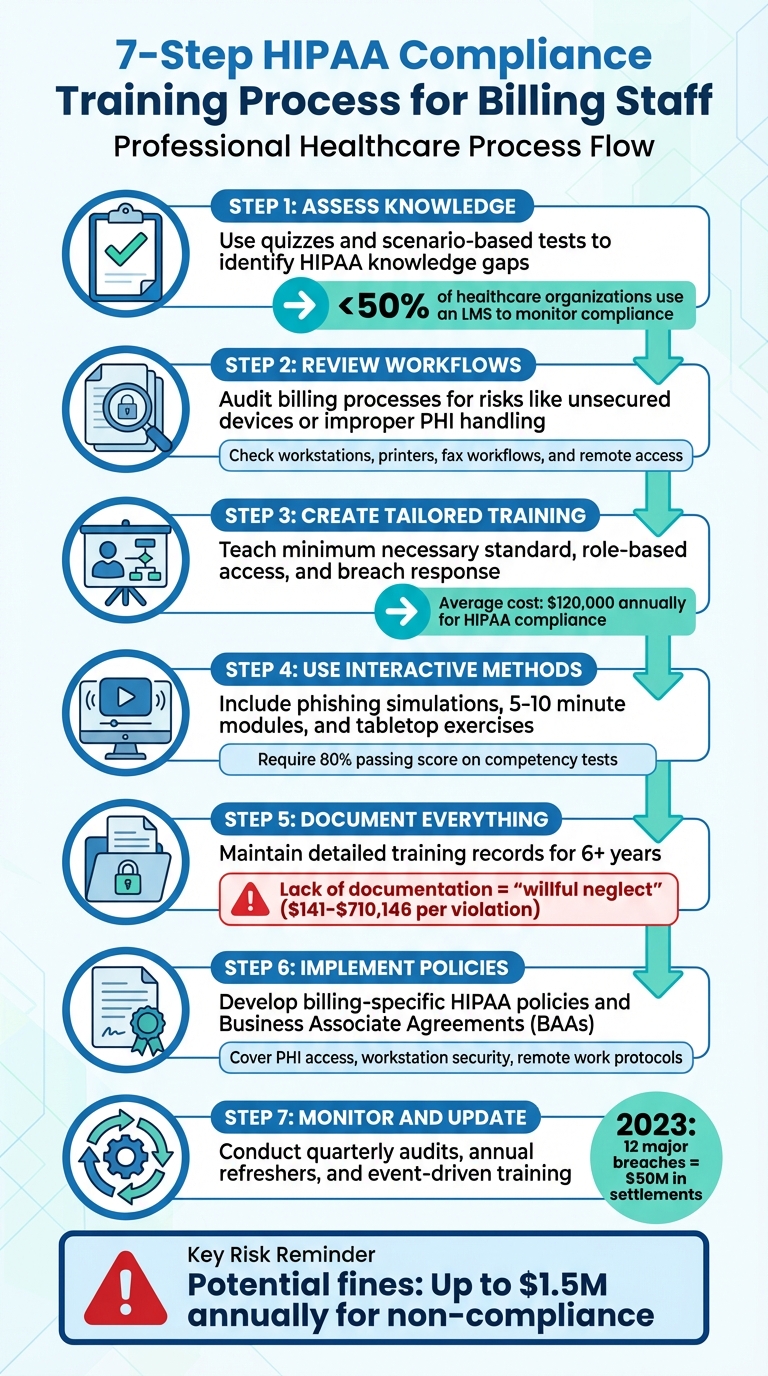
7-Step HIPAA Compliance Training Process for Billing Staff
Assess Current Knowledge and Identify Gaps
Start by evaluating your billing team's understanding of HIPAA requirements. Surprisingly, fewer than 50% of healthcare organizations use a Learning Management System (LMS) to monitor employee compliance. This suggests that many practices lack a clear understanding of their staff's HIPAA knowledge.
To address this, administer pre-tests and topic-specific quizzes that focus on the HIPAA Privacy, Security, and Enforcement Rules. Tailor these assessments to billing-related scenarios instead of generic clinical ones. For example, you can test knowledge of key HIPAA practices like applying the minimum necessary standard or verifying identities using two-factor authentication. Design the quizzes to provide instant feedback, turning them into quick learning opportunities for your team.
"A HIPAA training quiz converts passive learning into measurable proof that your team understands how to protect Protected Health Information (PHI)", says Kevin Henry, HIPAA Specialist at Accountable.
Conduct Baseline Knowledge Assessments
Scenario-based testing is an effective way to evaluate practical skills. Set up scenario labs where staff can practice tasks like redacting PHI, handling misdirected faxes, or responding to balance information requests. These exercises help determine if your team can apply HIPAA rules in real-world situations, rather than just memorizing definitions. Use the results to identify areas where operational processes need improvement.
Keep detailed records of all training activities. The Office for Civil Rights (OCR) views a lack of training documentation as "willful neglect", which can lead to violations during audits or breach investigations. For example, a Midwest physical therapy clinic faced a $35,000 settlement and a mandatory corrective action plan after an OCR audit revealed no formal documentation of HIPAA training, despite verbal claims of compliance.
These assessments not only pinpoint knowledge gaps but also provide a foundation for evaluating risks within your workflows.
Perform Workflow Risk Assessments
After identifying individual knowledge gaps, it's time to examine your billing workflows. Encourage staff to conduct self-audits of their workstations, printers, and fax workflows. Look for issues like unattended PHI, non-compliance with the minimum necessary standard, or improper handling of sensitive documents. A simple walk through the office can reveal risks, such as monitors facing public areas, unshredded PHI in recycling bins, or claim attachments left in printer trays. For remote billing staff, confirm they use secure VPNs, encrypted devices, and avoid printing PHI on personal equipment.
Also, review system audit logs to detect unusual activities, such as after-hours access, excessive data queries, or staff viewing records outside their assigned billing queue. These behaviors often signal confusion about role-based access rules. Additionally, assess how your team uses payer portals, manages EDI data integrity, and handles claim attachments. Identifying these gaps can reveal technical and administrative vulnerabilities in your processes.
sbb-itb-02f5876
Develop a Training Program
Once you’ve pinpointed knowledge gaps and identified workflow risks, it’s time to design a training program tailored to your billing team. Consider this: the average covered entity spends up to $120,000 annually on HIPAA compliance efforts. That’s a hefty investment, so your training needs to be effective. A tiered approach works well - start with a thorough onboarding program within the first 30 days, follow it with focused billing training over the next 60 days, and then schedule annual refreshers. This step-by-step method ensures your team gets the tools they need to stay compliant while keeping up with evolving regulations.
Key Topics to Cover in Training
Your training should cover both basic HIPAA principles and billing-specific scenarios. Start with the "minimum necessary" standard, which teaches staff to access only the PHI (Protected Health Information) they need for tasks like claims processing or appeals. Clarify when PHI can be shared with payers or business associates and emphasize key safeguards:
- Administrative controls: Role-based access, unique user IDs, and multi-factor authentication (MFA).
- Physical protections: Clean desk policies, screen privacy filters, and secure document shredding.
- Technical measures: Encryption for data in transit and at rest.
It’s equally important to train your team on patient rights, such as requests for access to records, amendments, or an accounting of disclosures. Breach notification procedures should also be a core focus. Teach your team to recognize warning signs like phishing attempts or misdirected faxes, and explain the internal reporting process. For breaches affecting 500 or more individuals, organizations must notify the Department of Health and Human Services within 60 days. In 2023 alone, 12 such cases led to nearly $50 million in settlement fees.
Use Interactive and Scenario-Based Training
To make the training stick, incorporate interactive methods. For example, run tabletop exercises that simulate breaches, such as a misplaced unencrypted laptop or a billing statement sent to the wrong recipient. These exercises help staff practice incident response in a controlled environment.
Short, focused modules - just 5 to 10 minutes long - can be especially effective for high-risk topics like phishing, secure messaging, or payer portal usage. Add gamification elements such as leaderboards or badges, and require competency tests with a minimum passing score of 80% to encourage active participation. Monthly lunch-and-learn sessions and timely updates after policy changes or near-miss incidents also help keep the team informed and engaged.
Use HIPAA-Compliant Tools Like Prospyr
Training is even more impactful when it’s tied to the tools your team uses daily. Prospyr, for instance, supports HIPAA compliance with features like encrypted data transmission, MFA, unique user IDs, and automatic session timeouts. It also tracks training activities digitally, reducing manual errors in billing workflows.
HIPAA-compliant tools like Prospyr simplify documentation too. The Office for Civil Rights views a lack of training records as "willful neglect". With digital tracking, you can automatically log who completed training, when, and on what topics - creating a solid audit trail for investigations. Prospyr can even flag unusual access patterns, triggering refresher training when needed. By integrating tools like this, you not only streamline daily operations but also reinforce your team’s commitment to HIPAA compliance.
Implement Policies and Documentation
Training alone isn't enough to safeguard your practice - you need written policies to formalize what your billing team has learned. These documents not only create a legal framework but also protect your practice during audits. The Office for Civil Rights requires clear, documented procedures, and failing to provide them can lead to "willful neglect" penalties ranging from $141 to $710,146 per violation. Your policies should outline how your team handles patient data, covering everything from claim submissions to payment posting. These written guidelines serve as the backbone for billing-specific safeguards, reinforcing the training your team has received.
Create Billing-Specific HIPAA Policies
It’s important to go beyond generic HIPAA guidelines by developing policies tailored to billing operations. These should formalize practices discussed during training, such as the minimum necessary standard, which ensures staff only access the PHI they need. For instance, billers might view payment data and claim details but shouldn’t access full clinical notes unless necessary for an appeal. A role-based access control (RBAC) policy can clearly define these boundaries, reducing the risk of unauthorized access. Documenting these rules helps ensure consistent enforcement.
Practical security measures should also be included. A workstation security policy might require screen auto-locking after five minutes of inactivity and enforce "clean desk" practices to prevent PHI from being left unattended, such as on printers overnight. For remote teams, a remote work policy should mandate the use of encrypted VPNs and prohibit printing PHI on personal printers. Additionally, a sanction policy should be in place to outline disciplinary actions for compliance violations, demonstrating to regulators that your practice takes these matters seriously.
"Understanding your business's unique needs is the first step; applying HIPAA guidelines to those needs is the next." - Emmy Kolbe, Copywriter, NY BillPro
To ensure everyone is on the same page, draft these policies in plain language so they’re easy for your team to understand. Require every employee to sign an acknowledgment confirming they’ve read and understood the policies. Keep these signed forms for at least six years, as HIPAA requires this retention period for all compliance-related documentation.
Establish Business Associate Agreements (BAAs)
Beyond internal policies, formal agreements with external vendors are essential for maintaining compliance. Any vendor that interacts with patient data must sign a Business Associate Agreement (BAA) before accessing any records. This includes your clearinghouse, cloud storage provider, billing service, and even practice management software. For example, Prospyr offers a BAA that outlines shared compliance responsibilities, such as data encryption, breach notification timelines, and procedures for secure data destruction after the contract ends.
"The cornerstone of HIPAA-compliant outsourcing is a comprehensive Business Associate Agreement (BAA)." - Medical Billers and Coders
A solid BAA should specify permitted uses of PHI, require safeguards like encryption under the Security Rule, mandate that subcontractors sign agreements, and define breach reporting timelines. It’s also vital to verify that everyday tools like Gmail (via Google Workspace) or scheduling software are covered by signed BAAs. Missing even one agreement could result in penalties exceeding $2 million annually for repeated violations.
Monitor, Test, and Provide Continued Education
Setting up policies is just the start - compliance is a continuous effort, not something you do once and forget. Without regular reinforcement, your billing team's knowledge can fade, and regulations are always evolving. The Office for Civil Rights expects organizations to actively monitor compliance and provide ongoing training, especially during audits.
"Even if you train your staff, if you can't prove it, it's as if it never happened." - Complydome
To stay on track with HIPAA requirements, it's essential to combine documented policies with regular audits and refresher training.
Conduct Regular Audits and Testing
Internal audits are critical for spotting problems before regulators do. Aim to perform workflow audits quarterly to uncover issues like unsecured files, outdated software, or employees accessing more PHI than necessary. For example, your billing manager should review role-based access levels every three months to ensure staff only have access relevant to their current job functions. A biller who transitions from claims submission to payment posting might still have unnecessary access to clinical notes.
Physical safeguards are just as important. Quick, 10-minute self-audits can help identify unattended PHI on desks, printers, or in recycle bins. Check that monitors are positioned away from public areas and ensure fax cover sheets display the correct recipient information before sending. These quick checks reinforce "clean desk" policies introduced during training. Use the audit trail from your initial training to track progress and identify gaps.
Tabletop exercises are another valuable tool. Walk your billing team through realistic breach scenarios, like sending a fax to the wrong recipient or losing an unencrypted laptop. Have them explain the steps they would take for notification and documentation. Track effectiveness metrics such as quiz results, phishing test outcomes, and how quickly staff report potential breaches. These metrics help you gauge whether your training is effective and highlight areas for improvement.
Schedule Annual Refreshers and Update Training as Needed
Regular audits should lead to periodic refresher training sessions to reinforce key policies and address any operational changes. While HIPAA doesn't specifically require "annual" training, 12-month refreshers are generally expected by auditors and insurers. For billing staff who work with PHI daily, consider offering bi-annual or even quarterly sessions.
Microlearning is a practical alternative to lengthy training sessions. Deliver short, focused modules - about 5–10 minutes each - on topics like secure messaging or proper media disposal. These can be done monthly or quarterly. This method not only meets HIPAA's "periodic" awareness requirement but also helps staff retain information more effectively than a single annual session.
Retraining becomes essential after major operational changes. For example, if you implement a new EHR system, add a telehealth platform, or switch clearinghouses, your billing team will need updated training soon after. Document every training session thoroughly, including course titles, dates, attendee names, quiz results, and signed acknowledgments. A Learning Management System (LMS) can simplify this process by centralizing records, sending automated reminders for overdue training, and tracking completion rates by department.
| Training Type | Frequency | Focus Areas for Billing Staff |
|---|---|---|
| Initial Onboarding | Within 10–30 days of hire | PHI basics, incident reporting, and workstation security |
| Annual Refresher | Every 12 months | Top violations, recent internal incidents, and policy updates |
| Event-Driven | As needed | New EHR modules, telehealth changes, or post-breach remediation |
| Microlearning | Monthly/Quarterly | Phishing awareness, secure messaging, and data disposal |
Conclusion
Creating effective HIPAA training for your billing team begins with understanding their current knowledge and builds through structured education and consistent oversight. Ensuring your team is well-prepared for HIPAA compliance is a continuous effort that protects both your patients and your practice.
Start by evaluating your team’s familiarity with handling protected health information (PHI) and identifying any knowledge gaps. Develop a comprehensive training program that emphasizes key principles like the "minimum necessary" standard, role-based access, and practical security measures - such as multi-factor authentication and clean desk policies. It’s also crucial to document all training sessions thoroughly. Proper documentation not only demonstrates compliance but also protects your practice during audits, as failure to do so can lead to costly penalties.
Regular audits, scenario-based exercises, and annual refresher courses are essential for maintaining compliance. These ongoing efforts help address human error, which is a common cause of HIPAA violations. Keeping detailed records of all training activities further reduces the risk of non-compliance.
HIPAA-compliant tools, such as Prospyr, can simplify this process by centralizing data and automating audit logs. A platform like Prospyr supports the training principles by offering a secure environment for patient data, enforcing role-based access, and maintaining automated logs. This eliminates the challenges of managing multiple systems and strengthens your team’s ability to handle PHI responsibly. By combining continuous education with tools like Prospyr, your billing team can confidently navigate HIPAA requirements while minimizing risks.
FAQs
What counts as PHI in billing?
PHI (Protected Health Information) in billing refers to any data that can identify a person and is connected to their health, treatment, or payment. This includes medical records, demographic details, insurance information, health-related dates, and contact details. It's essential to manage this information with care to ensure compliance with HIPAA regulations.
How do we apply the 'minimum necessary' standard in billing?
Applying the minimum necessary standard in billing revolves around limiting access, use, or sharing of protected health information (PHI) to what’s strictly needed for tasks like claims processing or payments. Billing staff should share only the PHI essential for completing these tasks. By establishing clear policies and safeguards, organizations can effectively restrict access to unnecessary information, ensuring compliance and safeguarding patient privacy.
What training records do we need to keep for HIPAA?
To comply with HIPAA, it's crucial to keep thorough records that prove your staff has been trained on privacy policies and procedures. These records might include certificates of completion, training logs, or documents detailing the training date, topics covered, and the personnel involved. Make sure every member of your workforce who handles PHI or ePHI is included in this documentation. Accurate and detailed records are essential for demonstrating compliance during audits or reviews.



